- 52shares
- Facebook1
- Twitter30
- Pinterest0
- LinkedIn20
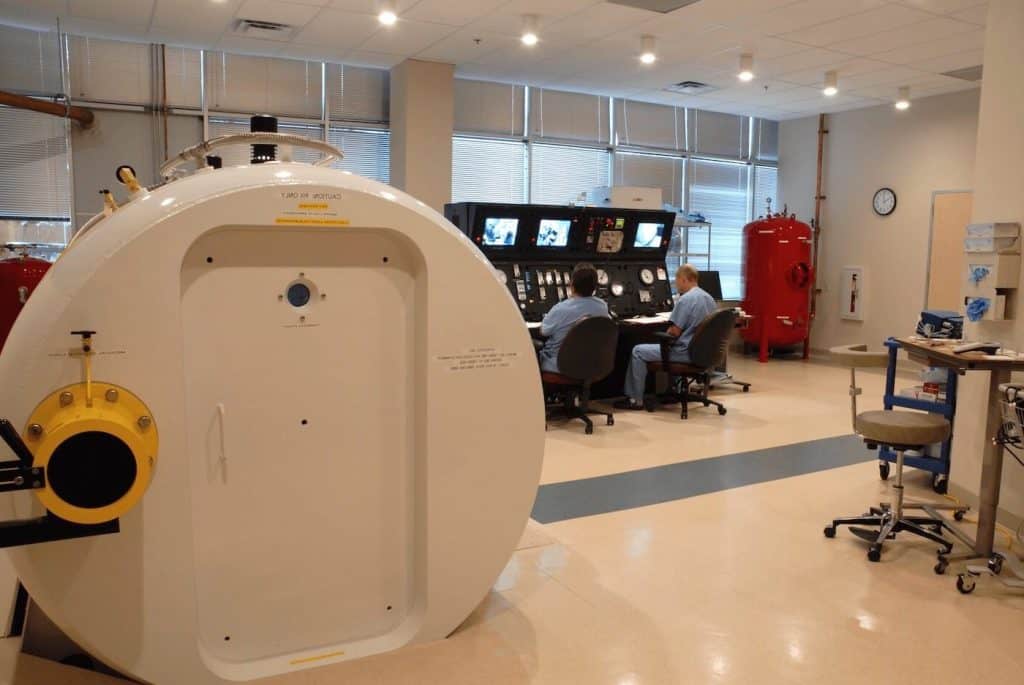
Hyperbaric Oxygen Therapy HBOT Risks
What is Hyperbaric Oxygen Therapy? HBOT is a prescribed treatment approved by the FDA and AMA in which a patient breathes 100% medical grade oxygen while the pressure of the treatment chamber is increased to a point higher than sea level pressure. This aides to speed and enhance the body’s natural ability to heal. HBOT is a safe, painless, non-invasive alternative and/or adjunctive therapy. Generally speaking, no serious complications are associated with Hyperbaric Oxygen Therapy, but some complications or side effects may be related to the primary condition treated.
Ear Barotrauma – Difficulty with clearing the ears causes “popping” and can cause mild to moderate pain. Middle ear barotrauma is the most common side effect of HBOT therapy. The patient prevents barotrauma by clearing their ears (equilibrating) during the chamber descent and ascent. A number of auto inflation maneuvers can be used, or, tympanotomy tubes can be used for those who cannot auto inflate.
Sinus Pain, Upper Respiratory Infections and Chronic Sinusitis – Sinus squeeze is seen less frequently than middle ear barotrauma. Antihistamines, decongestants, and/or nasal spray may be used prior to entering the chamber. With slow compression and decompression, usually there are no problems.
Myopia and Cataract – Myopia is a reversible complication of repeated exposure to HBOT. When progressive myopia does occur during a series of HBOT treatments, after completion of treatments, the visual acuity changes reverse completely. Acceleration of growth in existing cataracts is a complication of chronic long-term exposure at pressures over 2 ATA. Published reports as well as extensive clinical experience indicate that new cataracts do not develop within the series of 30 to 50 treatments that are commonly used in the USA.
Pulmonary – Pulmonary and neurological manifestations of oxygen poisoning are often cited as major concerns with HBOT. Oxygen tolerance limits that avoid these manifestations are well defined for continuous exposure in normal people. Pulmonary symptoms are not produced by daily exposure to oxygen at 2.0 or 2.4 ATA for 2 or 1.5 hours respectively. The incidence of oxygen convulsions when using similar exposure is about 1 per 10,000 patient treatments. Even when oxygen convulsions do occur, there are no residual effects if mechanical trauma can be avoided. Patients with airway obstruction have an increased risk for pulmonary barotrauma during decompression. Pulmonary barotrauma during decompression is rare.
Untreated Pneumothorax – The only absolute contraindication for HBOT is untreated pneumothorax. Surgical relief of the pneumothorax before HBOT treatment, if possible, removes the obstacle to treatment. A Chest x-ray may be necessary to rule out pneumothorax, if a patient’s medical history includes: 1) A history of spontaneous pneumothorax; 2) A history of thoracic surgery; or 3) A history of chest injury. Pneumothorax is a complication, which can be caused by breath holding during decompression.
Oxygen Seizures – Incidence of seizures is reported in 0.01% of 28,700 treatments and has never been reported at less than 2.0 ATA for an hour or less. Reference; Davis (1989) reviewed 1505 patients who were treated between 1979 and 1987 and underwent 52,758 two-hour sessions. Oxygen Convulsions occurred in only 5 patients, (0.009%) all of whom fully recovered.
Claustrophobia – Claustrophobia, which appears to be present in about 2% of the general population, may cause some degree of confinement anxiety. A mild sedative can be prescribed for those patients with anxiety.
Dental – All dental work, root canals, and fillings must be complete. Dental barotrauma is otherwise a possibility. Patients should not receive treatment if they have temporary dental caps or unfinished root canals.
References
Textbook of Hyperbaric Medicine, K.K. Jain, M.D., Vol. 1, 2, 3
Hyperbaric Medicine Practice, Eric Kindwall, M.D.
Care of the Patient Receiving Hyperbaric Oxygen Therapy, Manual of Patient Care Standards. 1988 Norkool, D
Hyperbaric Oxygen Therapy: A Committee Report 1999. UHMS
Fitness to Dive. DAN (Divers Alert Network)
UHMS (Undersea Hyperbaric Medicine Society)
IHMA (International Hyperbaric Medicine Association)
IBUM (International Board of Undersea Medicine)
NBDHMT (National Board of Diving and Hyperbaric Medical Technology)
We have an Expert waiting to Help You!
Make sure to carefully enter your Name, Phone Number, and Email Address and we will reply as soon as possible. Thank you!
- 52shares
- Facebook1
- Twitter30
- Pinterest0
- LinkedIn20
